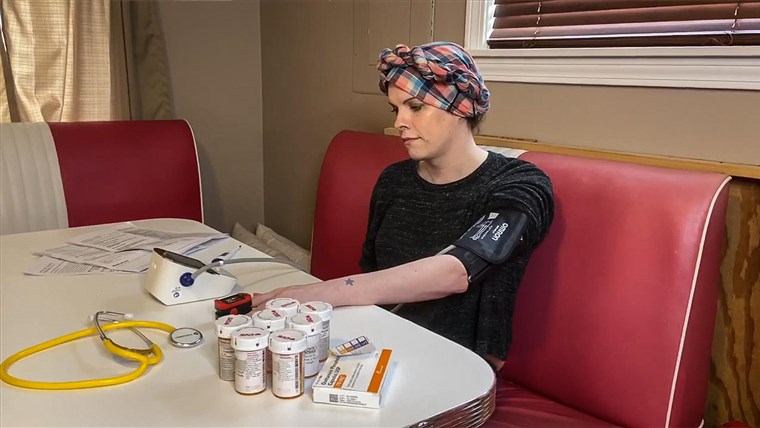
A 49-year-old man with asthma and obesity came into the hospital last month with COVID-19 pneumonia. His need for oxygen rapidly increased, so he was sent to the intensive care unit, where he was intubated and connected to a ventilator, and then hooked up to another machine for dialysis. Despite a tenuous course, he’s now getting better and is ready to leave the ICU.
It’s not just ICUs that are running out of beds; rehabilitation facilities are also short on space, staff and supplies.
His family is relieved he’s alive. The providers are, too — another life saved. But being stable enough to leave the hospital does not mean that this patient is well enough to resume his former life. Largely overlooked in the coverage of the devastation caused by the coronavirus is the fact that recovering from the disease and leaving the hospital are far from the end of the story.
After any ICU stay, and particularly the lengthy ones that accompany COVID-19, most patients need to go through rehabilitation before they can regain their former strength and functioning, if they ever do. And it’s not just ICUs that are running out of beds; rehabilitation facilities are also short on space, staff and supplies. We need to be paying much more attention to how COVID-19 survivors like this one are going to access the intensive rehab services they need to regain a meaningful quality of life.
The challenges start in the hospital, where COVID-19 survivors stay for between 10 to 13 days on average, and potentially months in the most severe cases. We’ve learned that patients often suffer from post-intensive care syndrome: Their muscles have atrophied after days of immobilization in a hospital bed; their lungs now struggle to provide oxygen to the bloodstream after relying on mechanical ventilators; their minds have become susceptible to delirium after disruptions to the brain’s supply of blood and oxygen.
Helping these patients return to normal requires early and dedicated access to a range of support services, such as physical and occupational therapy. Ideally, this road to recovery would begin in the hospital. However, COVID-19 patients in the ICU may still be contagious, and because many hospitals lack sufficient personal protective equipment to keep physical therapists safe from infection, they are often unable to treat anyone.
March 26, 202002:58
The roadblocks to rehab accumulate after discharge. Patients would normally be referred to a nursing home. But these facilities had little spare capacity prior to the pandemic, and some have resorted to evicting residents to accommodate the growing number of COVID-19 survivors. While the popular concept of a nursing home is that it is a place for the elderly to live, these facilities also serve as post-acute care providers for many patients requiring rehab.
Even when facilities have space, patients and their families might be reluctant to use them, given that these care sites have been hot spots for infection and accounted for nearly half of COVID-19 deaths in several states. Patients who do enter nursing homes will also need to be isolated to reduce the risk of infection to other residents, which coupled with restrictions on family visitations may exacerbate survivors’ psychological trauma from the ICU.
As an alternative, patients can request to receive rehabilitation services at home. However, recent research has found that home health agencies did not provide rehab for one-third of ICU survivors prior to the pandemic. COVID-19 has further exposed these challenges in the home health care industry, where supply chains are fragmented, agencies face shortages, and workers are consistently underpaid.
Gaps in personal protective equipment for home health aides are also concerning, as their generally older age and the high-touch nature of their work may increase their risk for COVID-19 infection. Consequently, both patient cancellations and staff absenteeism are on the rise. Although providers have advocated for the adoption of telemedicine to fill staffing gaps, virtual care alone is insufficient to meet the complex needs of recovering COVID-19 patients.
With caseloads rising and ICU death rates declining, a wave of COVID-19 survivors is forthcoming. While our understanding of the long-term effects of COVID-19 is still evolving, the emerging data coupled with evidence about ICU survivors in general suggest that gaps in rehab services may harm patients’ recovery in the short-term (such as by delaying their recovery) and long-term (by leading to a reduced quality of life).
Given that more than a quarter of hospitalized COVID-19 patients receive ICU care, the future strain on the health system may also be significant, with the risk of future hospitalizations and the potential added cost of long-term care. Consequently, policymakers need to act now to prepare the health system to meet the complex needs of these patients.
They need to start by shoring up our post-acute care capacity to ensure that all COVID-19 survivors receive the care they need on their journey to recovery. Authorities could consider repurposing community sites to build capacity and designate select health care facilities for COVID-19 patients to reduce infection risk. To increase the accessibility of home health, Congress should pass legislation to increase funding for home- and community-based services.
Providing safe care also requires addressing the medical supply shortage experienced by nursing homes and home health agencies. The United States should learn from Hong Kong where the implementation of minimum supply standards after SARS prevented virtually any COVID-19 deaths from occurring in nursing homes.
Additionally, we must ensure that it is safe for providers to deliver rehabilitation services. More than 4 million home, nursing and residential care workers were excluded from the emergency paid sick leave provided by the Families First Coronavirus Response Act to help Americans during the coronavirus crises. In the short-term, the Senate should join the House in passing the “Heroes Act,” which would close these gaps in paid sick leave and support workers’ capacity to physically distance. In the long-term, Congress should also pass legislation to recruit and train more direct care workers and guarantee them a living wage.
Gaps in rehab services may harm patients’ recovery in the short-term (such as by delaying their recovery) and long-term (by leading to a reduced quality of life).
Many COVID-19 survivors will likely experience the virus’s after-effects for years to come. Their experiences are a reminder of the need to strengthen the Affordable Care Act, such as the law’s protections for patients with pre-existing conditions. After all, the road to recovery is arduous enough without insurance coverage gaps and surprise bills.
We’re still learning about how best to treat the novel coronavirus. But it’s already clear that the battle doesn’t end with survival. We owe it to patients and their families to ensure that a return to normal physical routines and mental functioning is both possible and affordable.