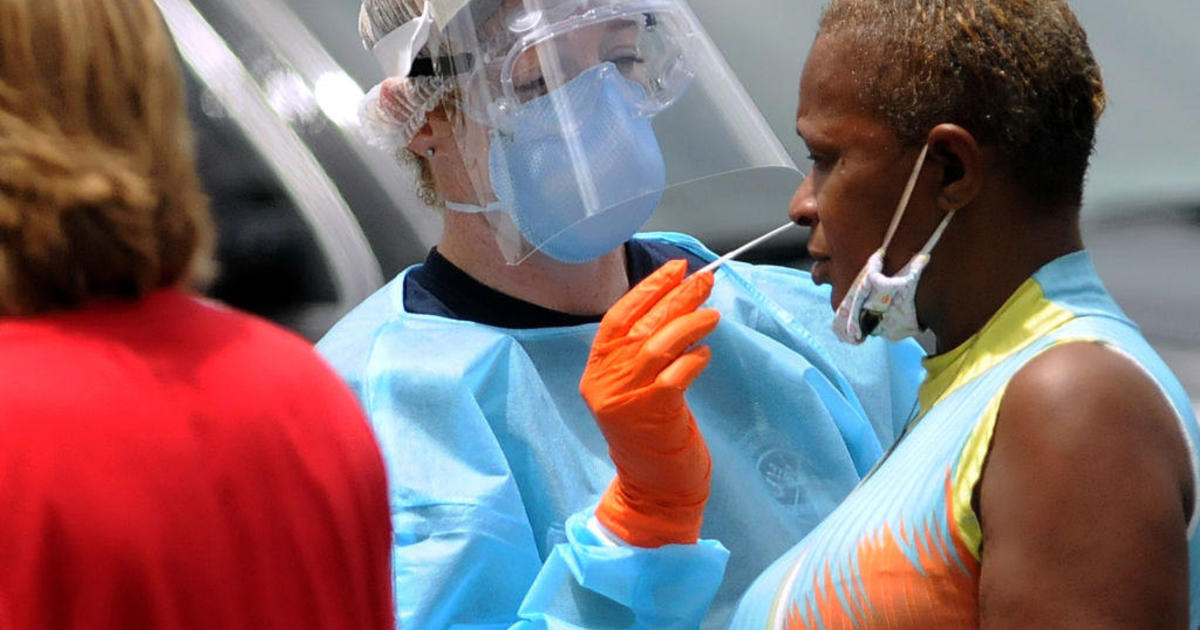
COVID-19 has disproportionately ravaged Black communities across America. Black Americans are three times more likely to die from the virus than Whites and more than 48,000 have died since the beginning of the pandemic. But as the U.S. moves closer to approving a coronavirus vaccine, public health officials are working to confront the long history of racism and mistreatment of Black Americans to sell them on a vaccine.
Studies suggest the Black community is “less inclined” to take the vaccine than any other racial group, according to a Pew Research Center study published this month. Of the 12,648 adults surveyed, only 42% of Black Americans would consider taking the vaccine, compared to 63% of Hispanics, 61% of White adults, and 83% of English-speaking Asian Americans who would.
The Black community’s distrust of the vaccine and the nation’s medical establishment is rooted in a long record of mistreatment. The late 1900s were defined by medical breakthroughs in the nation’s scientific community, but many of these experiments and discoveries were made at “the expense of Black people’s human dignity,” said Dr. Reed Tuckson, co-founder of the Black Coalition Against COVID-19. “There is a history of insults that have occurred in health care for people of color.”
In 1951, Henrietta Lacks, a woman suffering from cervical cancer, went to Johns Hopkins Hospital for treatment. When doctors took samples of her cancer cells, they discovered that her cells doubled at a rapid rate unseen before, making them ideal for cancer research. Since 1951, these “HeLa” cells, named after the first two letters in her first and last name, have been used to make advances in biomedical research.
But Lacks’ cells were used without her knowledge or consent and her family failed to receive any funds from the companies that used the “HeLa” cells to make medical discoveries.
Another infamous example: the Tuskegee Syphilis Experiment, a 1931 study conducted by the Public Health Service and Tuskegee Institute that examined the progression of syphilis in Black men.
In 1972, an Associated Press report revealed the hundreds of men participating were misled about the experiment and went untreated — even penicillin was withheld when it became the standard treatment for the disease in 1947. The men and their families were later granted a $10 million settlement and health benefits for their descendants from the federal government but the incident remains on the forefront of the Black community’s mind.
Earlier this week, Dr. Anthony Fauci said he fully respects the underlying skepticism of Black Americans but said it would be tragic for Black Americans to miss out on the benefits of the vaccines. “The terrible and shameful things that happened a long time ago are inexcusable,” Fauci said Tuesday. “It would be doubly tragic that the lingering effects of that prevent you from doing something so important.”
“The time is now to put skepticism aside,” Fauci said. “You’ll be saving yourself and your family illness, as well as that of your community.”
While these areas of distrust are historical examples, studies show Black Americans still face implicit racial bias and discrimination among health care providers. In underserved communities, Black individuals are less likely to have access to dedicated primary care doctors, a lack of health care that is directly linked to higher cases of chronic, unmanaged diseases in the Black community.
In Washington, D.C., Black residents make up roughly 46% of the population, but over 80% of virus deaths. In Chicago, Black residents died at six times the rate of White residents.
For twin sisters and doctors Delana Wardlaw and Elana McDonald, the lack of trusted Black doctors and poor primary care access in underserved communities are some of the biggest reasons the Black community is being hit hardest by COVID-19.
Poor or no access to regular healthcare can lead to a lack of diagnoses of chronic diseases, such as diabetes, asthma, high blood pressure, heart disease, and kidney disease — all conditions the CDC says puts people at greater risk for the virus.
Wardlaw and McDonald believe Black physicians can play an important and personal role in reducing the Black community’s fears and concerns about the COVID-19 crises, something they consider a “valuable” part of the education process.
The sisters established community COVID-19 testing in Philadelphia, where Black residents contract the virus at twice the rate of White Philly residents and make up over 55% of those hospitalized for COVID-19.
“The goal is to make sure that patients have adequate information, they are considering all the concerns, all the information and the options that are available so that we can make sure that we’re not allowing history to allow us to become a statistic,” said Wardlaw.
Even further, clinical trials for both the Moderna and Pfizer vaccines lack Black, Brown, and indigenous participants, as Black individuals make up only 10% and 8% respectively of their trial participants, a shortcoming that many in the Black community have cited as a reason for distrust.
Dr. Gary Gibbons, director of the National Heart, Lung, and Blood Institute at the National Institute of Health, said increasing the diversity of vaccine trials is essential to demonstrating trust to the Black community and ensuring the vaccine is effective for all people.
“It’s so critically important that the same communities that are so adversely affected by a disease, or in this case a pandemic, be included in the research designed to establish what is safe and effective, to more effectively treat or prevent this disease,” said Gibbons.
Around the country, Black health leaders, researchers, clergy, and advocates are working together to reduce the fears of potential vaccine participants. One such group: The Black Coalition Against COVID-19, has created a series of town halls directly addressing residents’ questions and concerns.
“It is our hope and conclusion there that by talking regularly and consistently with the Black community from a love-based, trusted and scientifically valid perspective, that we, in fact, should make a big difference in how many people are thinking about these issues and making choices and decisions for themselves, their families and their communities,” said Tuckson.
In New York City, the Ali Forney Center, a shelter dedicated to homeless LGBTQ+ youth, is working to stop the spread of misinformation surrounding the virus. The center recently transformed its education platform to focus on vaccine education.
“It’s especially important to note for this population, our young people have been let down by society,” said Alex Roque, the center’s director. “And if you lose that faith and when you lose that faith in the people who are supposed to love you, who do you trust after that?”
Ambrose Lane Jr., Chair of the Health Alliance, the largest community-based health advocacy group in Washington, D.C., said his group is working to educate Black residents on the vaccine. Lane said he is hopeful that renewed attention to medical distrust will help combat COVID-19 vaccine fears and the larger distrust of the nation’s scientific community.
“If we take this opportunity now to be able to really focus on addressing those disparities in our communities, we will have a better health care system and we will be prepared for the next time,” said Lane. “Because eventually, there will be a next time.”