So much of what I have reported on during the past year has been about the relentless march of the coronavirus around the globe and across this country, upending lives and economies. Now, being able to report on the first vaccines designed to protect us against the chaos and uncertainty, I am filled with hope.
That is why, when I was offered a chance to get vaccinated Friday morning, I jumped at it.
Because I am a high-risk health care worker, who — despite being on television most days — goes to the hospital on a regular basis to see and operate on patients, I am part of the first group of people to be offered the vaccine. I have to say, getting that shot felt like a profound and historical moment. And it didn’t hurt a bit.
But I didn’t make my decision lightly or blindly. I considered all the evidence. And because I did the homework, which I’ll outline here, maybe it will help address the vaccine concerns that some Americans have.
Tackling vaccine hesitancy
You might have noticed there is a little asterisk (*) after the word “hope” above. The asterisk — the footnote — is there because, for this promise of hope to be fulfilled, enough people have to agree to get vaccinated. Once that happens, our society will reach so-called herd immunity. That is, enough people will be immune to the virus, pushing down the infection rate. With fewer people to infect, the virus will gradually fizzle out and life can get back to normal — or settle into whatever will be the new normal.
Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, estimated that 75% to 85% of Americans would have to get vaccinated to reach herd immunity.
But we are not there yet. Vaccine hesitancy is real and it threatens this new, fragile hope for ending the pandemic as quickly as possible.
Dr. Susan Bailey, president of the American Medical Association, called vaccine hesitancy the biggest challenge remaining in the fight against Covid-19.
“Manufacturing, distribution, and administration still pose challenges, but the biggest threat remaining may be people’s willingness to get vaccinated,” she said in a statement Saturday, just as advisers to the US Centers for Disease Control and Prevention voted to recommend the Pfizer/BioNTech Covid-19 vaccine in the United States.
“To be clear, these vaccines will reduce death and severe illness. They have been rigorously evaluated, and if enough of us roll up our sleeves and get vaccinated, we can eventually reclaim normalcy,” she said.
Vaccine hesitancy is nothing new, nor is it particular to Covid-19 vaccines. Starting with the very first variolation efforts against smallpox in the 18th century, supporters had to convince skeptics that the practice helped more than it harmed. Most recently, gaps in vaccinations led to a global measles outbreak in 2019 that was felt acutely in the United States.
With respect to a Covid-19 vaccine, a Kaiser Family Foundation survey released this week found that 71% of respondents said they would “definitely” or “probably” get one if it were deemed by scientists to be safe and made free to the public — up from 63% in a September survey. That the numbers are increasing is good news.
But the Kaiser survey also found 27% of respondents said they “probably” or “definitely” would not get the vaccine, even if it were safe and free. Vaccine hesitancy is even high among some of the hardest-hit groups, who have the most to gain by the protection: 35% of both Black adults and rural residents say they “definitely” or “probably” would not get vaccinated, as do 33% of those deemed essential workers, and 29% of people who work in a health care delivery setting. Hesitancy is highest among Republicans (42%) and among people between the ages of 30 and 49 (36%).
The reasons behind this hesitancy vary. Between 50% and 60% of those surveyed by Kaiser cited concern over possible side effects, a lack of trust in the government to ensure safety and effectiveness, concern that these vaccines are too new, and concern over the role of politics in the development process; 43% believe the risks of Covid-19 are being exaggerated. Roughly half of hesitant Black adults say they don’t trust vaccines in general or that they are worried they may get Covid-19 from the vaccine.
Trust the science
I can’t address all the reasons for the hesitancy. I can only speak to the science behind the first two of these vaccines — one from Pfizer and BioNTech, granted an Emergency Use Authorization by the US Food and Drug Administration last week, and the other from Moderna, which was given an EUA Friday.
First and foremost, I reviewed all the safety data — because when it comes down to it, a vaccine is meant to prevent illness. And right now, I’m healthy. The last thing I want to do is take something that makes me sick. There was a lot of back and forth on just how much safety data would be required for an EUA. What was decided was two months of safety data would be needed, because most adverse events occur within 42 days. And it turns out, both vaccines have safety profiles that are favorable.
Could there be adverse events that appear after two months? Yes. Could there be unexpected side effects when you give shots to tens of millions of people instead of tens of thousands? Also yes. We saw that recently with at least five vaccine recipients developing severe allergic reactions. But overall, the potential good outweighs the possible harms.
Don’t confuse serious adverse events with the expected side effects of getting the shot. About 10% to 15% of vaccine recipients can expect to experience side effects such as headache, arm pain, fatigue and fever, according to Operation Warp Speed Chief Scientific Adviser Moncef Slaoui. These will all clear up after a day or so. It shows the vaccine is doing its job — preparing your immune system to fight against the coronavirus.
Maybe the most stunning thing about these two vaccines — which both rely on new mRNA technology — is how well they work across age, racial and ethnic groups. It’s incredibly reassuring to think that once you receive your two shots, you’re about 95% protected against a disease that has had many of us worried for almost a year now. It’s like having personal protective equipment at a molecular level.
In the Phase 3 clinical trial of the Pfizer/BioNTech vaccine, more than 40,000 participants received either two doses of the vaccine or two doses of a placebo. Of the 170 cases of Covid-19, 162 were in people who got placebo, while eight cases were in participants who got the actual vaccine. Among the 10 severe cases, only one occurred in the vaccinated group. The vaccine was found to work equally well across age, race and ethnicity demographics.
In Moderna’s Phase 3 trial, 15,000 study participants were given a placebo, and another 15,000 were given the vaccine. Of the 196 cases of Covid-19 that emerged, 185 of them were in the placebo group — 30 of them severe, including one death — compared to only 11 cases in the vaccine group. This vaccine, too, was found to be effective across age, racial and ethnic groups.
Full transparency
In addition to understanding the remarkable benefits of these two vaccines and being satisfied with their safety profile, I also had the privilege of interviewing most — if not all — the major players who’ve had roles in the development of these vaccines, from Operation Warp Speed’s Slaoui, to US Health and Human Services Secretary Alex Azar and Assistant Secretary for Health Admiral Brett Giroir; from Fauci, possibly the country’s best-known infectious disease expert, to FDA Commissioner Dr. Stephen Hahn, whose agency authorizes or approves vaccine candidates; from Dr. Barney Graham and Kizzmekia Corbett, co-developers of the Moderna vaccine, to Albert Bourla, CEO of Pfizer.
They all stand behind the science of the vaccines and have stated repeatedly that no corners were cut, and that politics did not play a role in their processes.
“These are the product of an independent, safe system — some of the largest vaccine clinical trials in history,” Azar told CNN’s Jake Tapper and me on “The Lead” Monday. Azar was speaking from George Washington University Hospital, where some of the first shots were being administered.
“The best thing that we can do is ensure the rigor and integrity of the process, and then the transparency of the data,” Azar said. “We want to make sure, especially in those medically underserved communities, especially the racial and ethnic minorities that have suffered so much at the hands of this virus, that we increase vaccine confidence by having trusted voices out there who will assure the community that these are vaccines that are safe and effective.”
And that brings me to the following statistic. Both vaccine makers were told by the FDA to ensure their trials enrolled at least a proportionate number of participants from hard-hit, minority communities. The result is that approximately 30% of each trial’s volunteers are Black or Hispanic.
The National Institutes of Health’s Corbett, who as lead scientist for coronavirus vaccine research was one of the Moderna vaccine co-developers, says she, as a Black woman, knows that attitudes in minority communities won’t change overnight.
“The first step is … to understand that the onus of this problem is not on them and their distrust. It is on us and our level of trustworthiness. And so, trust, especially when it has been stripped from people, has to be rebuilt in a brick-by-brick fashion. And so, what I say to people, firstly, is that I empathize. And then, secondly, is that I’m going to do my part in laying those bricks,” she said recently on my podcast, “Coronavirus: Fact vs. Fiction.”
And the surveys show those attitudes are beginning to change.
That same Kaiser Family Foundation poll showed that not only has willingness to get a Covid-19 vaccine gone up — from 50% in September to 62% in December among Black respondents, and from 60% to 71% among Hispanics — but also that confidence in the testing process has also gone up: 67% of Black respondents and 61% of Hispanic respondents said in December they are very or somewhat confident that a vaccine will have been properly tested for safety and effectiveness, compared to 39% and 51% who felt that way in September.
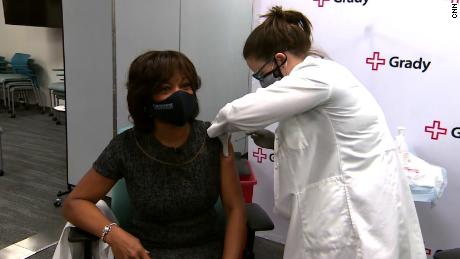
When I got my vaccine, I was joined by my colleague, Dr. Valerie Montgomery Rice, president and dean of Morehouse School of Medicine.
“What we know that’s different now is that there are Black scientists in the room where the decisions are being made. There are Black scientists who (are) in the development of the vaccine. There are Black scientists who are on the FDA advisory panel. There are Black scientists on the (CDC’s Advisory Committee on Immunization Practices). There are Black scientists on the CDC advisory boards,” she told me.
“And then there are people like me, who are looking at the data, helping to interpret it, working with the National Academy, giving our recommendations of the allocation. So, we’re in the rooms where it’s happening. So, we clearly are not going to go against ourselves … because we understand how critical this is for Black America and Latinx America, who have been disproportionately impacted by the virus. I would not actually recommend anything if I did not believe it was safe,” she said.
And if you still have questions, seek out answers.
“Ask your doctor if you have questions,” US Surgeon General Dr. Jerome Adams said during a news conference at George Washington University Hospital on Monday. “Don’t let misinformation be the reason you aren’t getting everything that you deserve to be your healthiest self.”
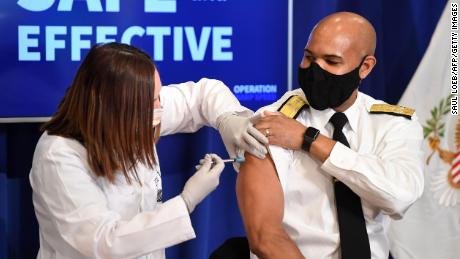
Like Montgomery Rice and me, Adams got his first shot on Friday too, along with the Vice President and the Second Lady.
Like soldiers who were killed after the armistice
The newest model out of the University of Washington’s Institute of Health Metrics and Evaluation projects nearly 250,000 additional Americans will die from Covid-19 by April 1 of next year. That’s on top of the more than 310,000 who have already succumbed to the disease.
It’s important to remember the vast majority of those people feel fine right now; they’re not sick. But at some point over the next four months, they’re going to become infected; some are going to get really sick and they’re going to be surprised by that. And a small percentage will die.
The same IMHE model also predicts that a new coronavirus vaccine could save 20,000 or more lives. But that’s only if people are willing to take it. That’s why I think not taking a vaccine when it’s your turn and you have the chance could be a missed opportunity. It’s like the 3,000 soldiers who died in World War I between the signing of the armistice and its enactment six hours later.
It would be a real tragedy to be taken down in sight of the finish line.